An Overview
There are two main objectives in treating periodontal disease. The first goal is to reduce and control the bacterial colonies that form under the edge of the gum. The second goal is to eliminate any known factors that cause the patient to be more susceptible to breakdown. Primary among these is smoking.
In the early stages of periodontal disease (gingivitis), the gum is infected but the bone has not yet been altered. The pocket depth is generally only slightly deepened, to 4-5 mm. Scaling and root planing ("deep cleanings") are done to remove any calculus that has formed. If the pockets are tender, numbing the gums is often necessary so there will be no discomfort during the procedure. There is little or no pain afterward. The patient must keep plaque from reforming by daily brushing and flossing. The healing gum will snug back up around the root, and health will return. Daily plaque removal with regular dental cleanings will prevent a reoccurrence.
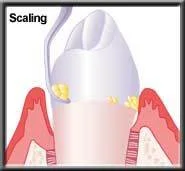
Scaling removes plaque & calculus
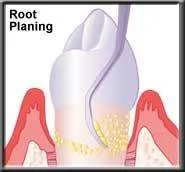
Root planing smoothes the root surface
In a few cases, the swollen gums may not shrink back to normal after the infection is removed, and must be trimmed by the dentist with a gingivectomy. Otherwise the swollen gum makes removal of plaque by the patient impossible, and the problem starts again.
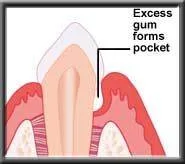
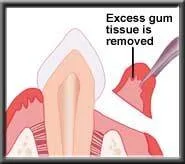
Pocket reduction with a gingivectomy
In more moderate cases, there is actual bone loss, and the pockets may be 5-7mm in depth. Scaling and root planing will not predictably remove all the calculus from these deeper pockets, because of limited and difficult access in reaching the bottom of the pocket. In these cases flap surgery is needed so the periodontist can gain access to clean the root. With this procedure, an incision is made between the gum and tooth, and the gum is peeled back away from the neck of the tooth and the edge of the bone. The surgeon can then easily see the deep calculus, and adequately debride the tooth.
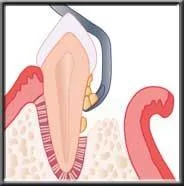
Flap reflected to access deep plaque and calculus
After flap surgery the tissue may be returned to its former position, which minimizes cosmetic changes. However, because the gum can not connect back to the tooth, this does not eliminate the pocket. With the pocket remaining, the patient cannot remove all the bacteria, and must rely on frequent hygienist cleanings to help control reoccurrence of the infection.
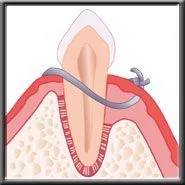
Flap returned to normal
The ideal flap surgery, pocket elimination surgery, is achieved when the periodontist surgically removes the pocket by repositioning the gum down to the new bone level. Any irregularities or pitting of the bone that was caused by the infection is first corrected, and the gum is sutured tightly down to the re-contoured bone. This pocket elimination allows the patient to access and remove the bacterial plaque daily with brushing and flossing. If all plaque is eliminated daily, the disease is completely arrested.
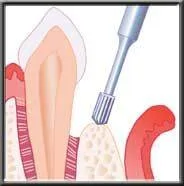
Pitted bone re-contoured during osseous surgery
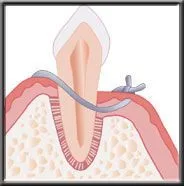
Flap sutured tightly down to recontour bone
Pocket elimination surgery can cause cosmetic changes around the upper front teeth, and the periodontist may avoid pocket elimination surgery in this area to minimize any changes that could be seen.
If surgery is necessary, the main scaling and root planing is often done at the surgery, rather than before. During surgery the periodontist can see and reach all areas, allowing for better tooth cleansing. However, each case is treated according to need and in cases where the need for surgery is not certain, the non-surgical scaling and root planing is performed first. The patient is then re-evaluated to see if further treatment is required.
In advanced cases, there has been extensive bone loss, and pocket depth may be 8mm and more. In these cases complete removal of the pocket is often not possible, due to limitations on how far the gum can be moved. However, surgery is necessary for the periodontist to access and clean the deeper areas, which cannot be effectively scaled without reflecting the gum. The objective is to thoroughly cleanse the roots, and to reduce the pockets as much as possible. Antibiotics may be prescribed to help eliminate very aggressive bacteria.
In the last decade there has been much research in actually re-growing the bone destroyed by periodontal disease. While not effective in all cases, today many periodontal lesions can benefit from these regeneration procedures. Your periodontist will tell you if you are a good candidate for regeneration. (See Regeneration)
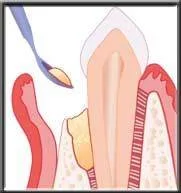
Placing synthetic bone
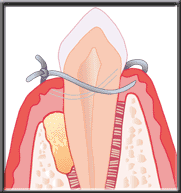
Synthetic bone placed in defect

Synthetic bone stimulates patient's natural bone to regenerate
In cases where surgery is not, or cannot, be performed, or in very advanced cases, there are often residual pockets after treatment. The deeper these pockets, the more guarded the long term results will be. We try to reduce pockets as much as we can. As a rule of thumb, the shallower the pocket, the better the chances of maintaining the tooth. With a shallower pocket the hygienist is able to clean more thoroughly at recall appointments, and the patient is able to remove a greater percentage of the plaque that forms.
Periodontal disease may be considered a chronic disease, and for that reason a complete "cure" is usually not possible. Patient susceptibility may continue to be high, and the cause of infection, plaque, is always present in the mouth. Daily vigilance is needed to control the disease and keep the gums in good health. Even with the best care certain areas may lose ground, although the vast percentage of patients who follow good maintenance can expect to have their teeth for their lifetime.
In summary, the treatment of periodontal disease focuses on removing bacterial plaque and calculus that forms under the gums. In more severe cases surgery is used to provide access for scaling, and to reduce pocket depth so the patient can more effectively access and remove plaque from their teeth at home. Good oral hygiene along with regular periodontal maintenance ;appointments (recalls) will help preserve the teeth for a lifetime.